
health
Everything you need to know about Black fungus
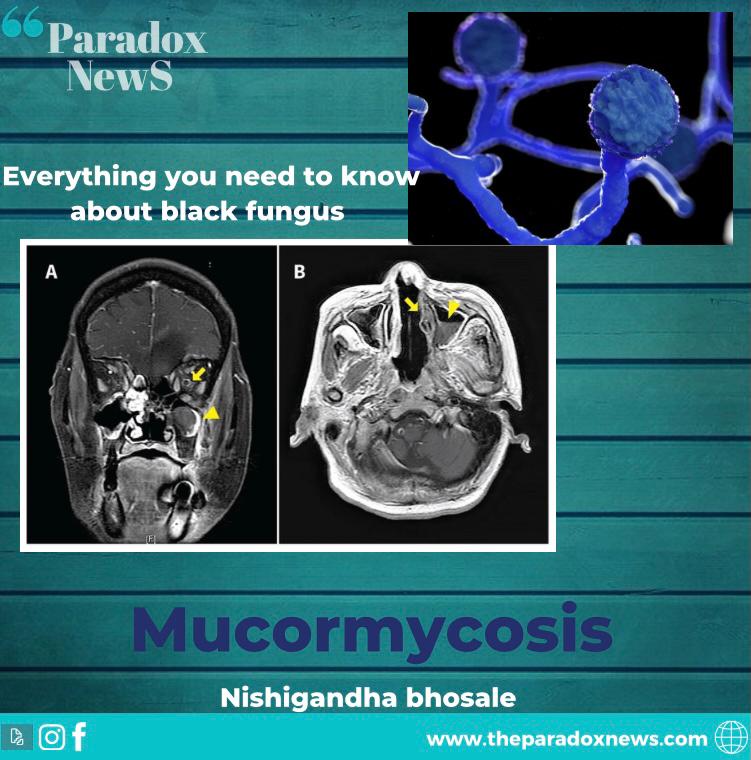
Mucormycosis: The Black Fungus
COVID-19 and The Black Fungus (informally referred to as The Black Fungus) is the new lethal complication.

• India is combating the deadly second wave of coronavirus and lately, such potentially deadly complication is being observed in patients recovering from COVID-19 all over the country and this has increased the tensions.
• Being a medical student, I’d like to elaborate this topic, and share a bit of information I have and let the plebs out there understand this in quite a simple way.
• What is mucormycosis and it’s cause?
(previously termed zygomycosis)
Mucormycosis is any fungal infection, non-contagious, typically caused by a group of molds called mucormycetes or by a fungi in order Mucorales. Can be fatal if left unattended. Mucoralean fungi are the first colonisers of dead or decaying plant material.
• There are several types of mucormycosis such as Rhinocerebral Mucormycosis, Gastrointestinal Mucormycosis, Pulmonary (lung) Mucormycosis and Cutaneous (skin) Mucormycosis and Disseminated Mucormycosis.
But the most common one, which is found in the COVID-19 patients is the Rhinocerebral Mucormycosis. The overall mortality rate is approximately 50% that rises to about 85% in Rhinocerebral Mucormycosis. There is no vaccine to prevent mucormycosis.
• What are the sources of this fungus?
Common sources of infections are from soil, damp walls on old buildings, decaying organic matter.
Recently mentioned source, that only distilled water should be used for hydrating oxygen, sometimes tap water, or any other available water, is being used either due to ignorance or negligence.
• How is it medically diagnosed?
Presumptive diagnosis is based on the patient’s history and physical examination.
Tests such as CT or MRI help defining the extent of infection or tissue destruction.
• Who’s at higher risk?
Not all people having COVID-19 obtain mucormycosis, but the most prone to getting affected may be:
- People taking immunosuppressant steroid medications to manage pre-existing illnesses as well as COVID-19, over a long period of time. Because steroids reduce immunity and push up blood sugar levels in both diabetics and non-diabetic patients.
- Prolonged ICU stay.
- People having weakened immune system because of previous organ transplant surgeries or cancer therapy procedures.
- People with HIV/AIDS, congenital bone marrow disease, diabetes mellitus are prone to developing mucormycosis.

• What are the common symptoms?
- Headache
- Fever
- Dark scabbing in the nose and by the eyes
- Necrotic black lesions on the hard palate
- Unilateral facial swelling or near cheekbones,
reddish skin over nose - Sinusitis: nasal clogging or congestion with bloody or blackish mucus discharge
- Hazy vision: objects appearing blurred or in double
- Tooth ache, or pain in jawbone
- Abnormal blood clotting or thrombosis
- Black pus from eyes in case of periorbital infection.
• What should be the obvious treatment?
Once diagnosed, urgent medical care by a team of specialists including a microbiologist, internal medicine expert, neurologist, ENT Specialist, ophthalmologist, dentist should be given. It must be fast and aggressive, because the tissue damage caused cannot be reversed.
- Antifungal medications: Amphotericin B given intravenously is the usual drug of choice. Lipid formulations of amphotericin B are often used as first-line treatment.
Also, posaconazole or isavuconazole may treat mucormycosis can be given orally too. - Surgical debridement of the infected area.
• What are serious complications?
- Blindness: in case of periorbital infection where eye is affected and vision is lost.
- Meningitis: inflammation of the membranes (meninges) that surround the brain and spinal cord.
- Pulmonary hemorrhages.
- Brain abscesses.
• Is it possible to prevent Mucormycosis?
- Good control or treatment of health problems with diabetes.
- Ensuring personal hygiene.
- Wearing face masks, face shields, gloves and all protecting equipments.
- Patients recovering from COVID-19 should stay indoors and should take extreme care.

-

 Fashion6 years ago
Fashion6 years ago4 more clicks please!
-

 Entertainment6 years ago
Entertainment6 years agoDisha Patani is a National crush and Why?
-

 Paradox recommends6 years ago
Paradox recommends6 years agoWAJID KHAN song list forever in heart and on the playlist
-

 Fashion6 years ago
Fashion6 years agoWhen sonam kapoor gave us major princess goals.
-

 Interview5 years ago
Interview5 years agoMadhura Joshi Divekar tells us her story, passion and more.
-

 Entertainment5 years ago
Entertainment5 years agoBest bollywood villains of 90s and the iconic actors.
-

 Food6 years ago
Food6 years agoTerrace Farming- A clever way to grow greens.
-

 Entertainment6 years ago
Entertainment6 years agoOUR CELEBRITY BRIDES!
-

 Interview5 years ago
Interview5 years agoTirth Parsana: one who gives a laughter pill
-

 Business6 years ago
Business6 years agoElon Musk : undaunted visionary character shaping our future
3 Comments